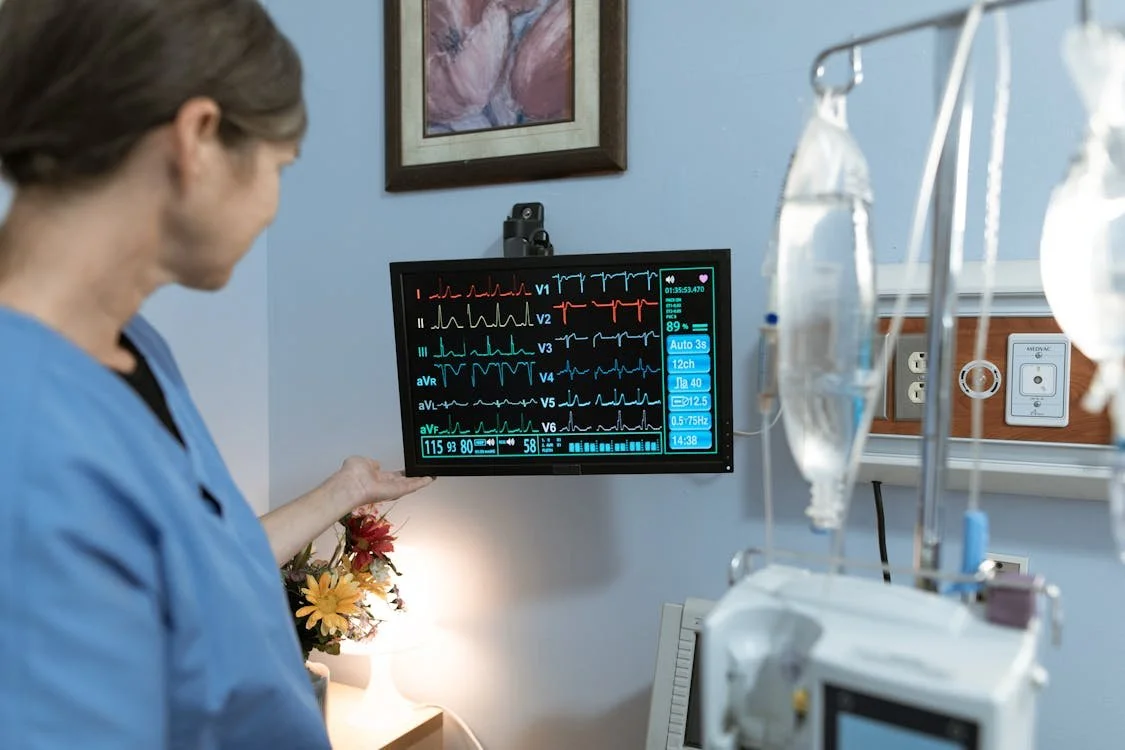
What Really Happens in the Recovery Room After Surgery?
Most people put all their energy into preparing for the surgery itself. The night before, the drive there, what to bring, what the surgeon is going to do. What almost no one prepares for is what happens in the first hour after — and the recovery room can feel disorienting, even frightening, if you don't know what to expect.
I've spent years in surgical units and in same-day surgery, and I've watched patients come out of anesthesia confused and scared because no one told them what waking up would feel like. That's not how it should go. You deserve to walk into surgery day with a full picture, not just half of one.
Here's what the recovery room is, what your nurses are doing while you're there, and what's normal — even when it doesn't feel like it.
What You'll Learn
- What the recovery room is and what your nurse is watching while you recover from anesthesia
- What waking up from surgery actually feels like — and what's normal
- What families can expect during this time, since they usually can't be in the room
What the Recovery Room Actually Is
The recovery room — you'll hear it called the PACU, which stands for post-anesthesia care unit — is a specialized area of the hospital or surgical center where patients are monitored closely as anesthesia wears off. The nurse-to-patient ratio here is intentionally much lower than it is on a regular hospital floor, often one nurse for every one or two patients. That's by design. The first hours after surgery require close, continuous attention.
You won't be in a private room. Recovery rooms are often open-plan spaces divided by curtains. There will be monitors attached to you — tracking your heart rate, blood pressure, and oxygen levels. Your nurse will be checking on you frequently, sometimes nearly constantly in the first few minutes after you arrive. This is exactly what should be happening.
What You Might Feel Coming Out of Anesthesia
This is the part most patients aren't prepared for, so I want to be specific.
Confusion is normal. Anesthesia affects people differently, but most patients feel groggy and disoriented when they first wake up. You may not remember where you are for a moment. You may feel like you've been asleep for days even if the procedure was two hours. That fog lifts as the anesthesia clears your system, but it takes time, and it's not something you can rush.
You may feel cold or start shivering. Operating rooms run cold, and your body temperature often drops during surgery. Many patients wake up shaking. Your nurse will bring warm blankets, and shivering usually resolves within thirty minutes or so. Let them know if you're still cold.
Nausea can happen, and it's treatable. Some people are more sensitive to anesthesia than others, and nausea is one of the more common effects in recovery. If you feel nauseated, tell your nurse right away. There are medications that work quickly, and there's no reason to wait it out. The same goes for pain — tell your nurse when you're hurting. Managing both of these things in the recovery room is part of the plan, not a burden.
A sore throat is common. If you had general anesthesia, a breathing tube was placed during surgery to keep your airway open. A mild sore throat or dry mouth afterward is normal and usually clears up within a day or two.
What Your Nurse Is Doing While You Recover
Your recovery room nurse is doing a lot while you're waking up. They're checking your vital signs every fifteen minutes or more often, monitoring your oxygen levels, watching your pain level, and keeping an eye on any signs that need attention — a drop in blood pressure, difficulty breathing, bleeding beyond what's expected. They're also checking that you're alert enough and stable enough to move to the next phase, whether that's a hospital room or, for same-day procedures, home.
When patients or families describe the recovery room, they often say it felt like a long time. That's partly because the clock moves strangely when you're groggy, and partly because there's genuinely not much to do but wait. Your body is doing the work. The nurse is watching it happen.
What Family Members Should Know
In most hospitals and surgical centers, family members can't be in the PACU. This is one of the hardest parts of surgery for families — your loved one is out of the operating room but you still can't see them. That wait is real, and it's hard.
The reason isn't bureaucratic. The recovery room is a high-monitoring environment where nurses need to work quickly and without distraction at key moments. Once your loved one is stable and moved to their room or ready for discharge, you'll be brought back in right away.
If you haven't heard anything within the time your surgeon estimated, ask the waiting room staff for an update. You don't have to sit silently. And if you're helping an elderly parent or a spouse through this, staying in the waiting room and staying calm is genuinely useful — it means you're ready and present when the nurse comes to get you.
Coming out of anesthesia isn't a graceful process, and it doesn't have to be. Your job in that first hour is simply to let your body do what it needs to do. Tell your nurse what you're feeling. Accept the warm blanket. Take the anti-nausea medication if you need it.
And to the family members in the waiting room — you're doing the right thing by being there. That matters more than you know.
Shira Graham, RN, BSN is a patient advocate with 34 years of nursing experience.
Shira's Patient Advocacy Services was created to help patients and families navigate the healthcare system with confidence.